Understanding Social Determinants of Health SDOH and its Integration With Health Equity
Do you know what social determinants of health SDOH stands for? Sure, you must know, however, when you seek to improve health in the USA we overlook SDOH social determinants of health and consider looking at the healthcare system only. However, the reality is that nearly 66% of Medicaid recipients are currently registered in risk-based managed care schemes across the country. This data clearly shows that SDOH and health equity are a must for solving mental disorders in the long run.
To help healthcare providers understand what social determinants of health SDOH are, and how to address mental health disorders with an effective SDOH health strategy, we’ve compiled a quick guide that will surely help the healthcare payers to make an informed decision. So, without any delay, let’s learn more about SDOH and health equity and improve the members’ overall well-being.
What Are Social Determinants of Health SDOH?
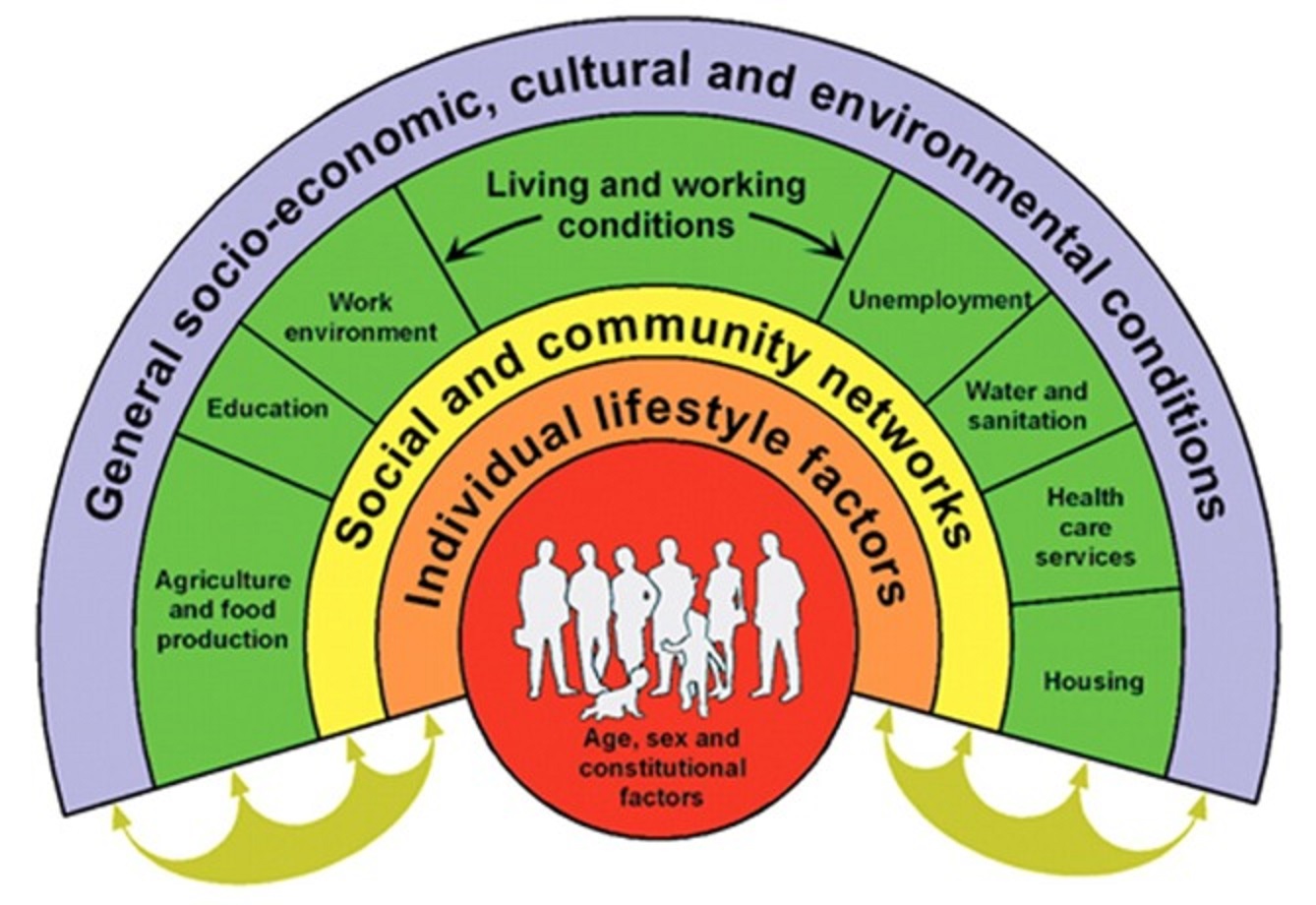
The World Health Organization (WHO) Trusted Source defines social determinants of health SDOH as “the conditions in which people are born, grow, work, live, and age, and the wider set of forces and systems shaping the conditions of daily life.”
In simplest terms, SDOH social determinants of health are factors that affect the mental health and the overall well-being of an individual’s personal life.
As outlined in Healthy People 2030, the fifth edition of a set of science-based, 10-year national objectives developed under the U.S. Department of Health and Human Services, SDOH health can be grouped into five domains.
Five Domains of SDOH Social Determinants of Health
-
Healthcare
This group includes an individual’s ability to receive healthcare and the standard of care received. Some key elements of this group consist of accessibility to basic healthcare, having health insurance, and understanding health information.
-
Economic Stability
This group encompasses a link between a person’s finances and their health. Examples of these are – poverty, employment, food security, and housing stability.
-
Education
This category focuses on the connection between a person’s access to education and its quality, and their health. Some examples of these include – secondary education, higher education, language and literacy, and childhood development.
-
Social and Community Life
This group revolves around the ways a person lives, works, plays, and learns and how these relate to the person’s health. Some examples of these include – civic participation, discrimination, and incarceration conditions within a workplace.
-
Neighborhood
This group considers a person’s housing and environment and the role they play in the person’s health. Some examples of these are – quality of housing, transportation, access to healthy foods, water quality, and crime and violence.
The above factors in each group are interwoven and often related to each other. Now, that you know what social determinants of health SDOH mean and what are its 5 heads, let us know how social determinants of health SDOH impact mental health care.
How Does SDOH Health Impact Mental Health Care?
In today’s time, mental health and disorders are a big concern among people of any age. Though mental health can harm everyone irrespectively, still it is seen that mental health disorders among children and teenagers can lead to a variety of negative outcomes, including:
- Failure in school
- Family conflict
- Violence
- Alcohol or drug abuse
- Suicide
Though these above social determinants of health SDOH can impact mental health care badly, healthcare providers using the social determinant interventions can solve this critical issue. Yes, by using proper and strategic social determinant interventions the healthcare payers can provide their patients with better mental health outcomes.
However, tracing the connections between individual mental health and SDOH social determinants of health can be tricky. To help the healthcare payers on this, we’ve highlighted a few major steps that can effectively help to trace the problems and improve overall well-being.
Top 4 Strategies for Healthcare Payers For Integrating SDOH and Health Equity for Improved Mental Health Outcomes
-
Understanding Social Determinants of Health SDOH
The first step healthcare payers can take to improve the overall mental health of their patients is to understand the social determinants and know what populations may be more vulnerable to these social determinants than others. The following are some SDOH social determinants of health that impact mental health care.s
- Age
- Race
- Ethnicity
- Gender
- Education level
- Income level
- Geographic location
- Quality of housing
- Interpersonal and community dynamics
- School and work conditions
- Employment opportunities
These factors can have negative or positive effects on mental health and risk. While an impoverished area with a high crime rate can hurt mental health, safe shared spaces like parks can promote positive mental health.
-
Analyze SDOH Data for Comprehensive Member Understanding
The second step requires understanding the combination of SDOH and health equity. Health plan providers must recognize that SDOH health is the foundation of providing whole-person care. At the current time, the process for identifying and addressing SDOH health can be reactive. In other words, healthcare payers may not realize a member is considered high-risk or high-cost until they have visited the emergency department several times.
To understand and eradicate the member’s high-risk or high cost, the healthcare payers can lower costs and promote holistic care by conducting SDOH health assessments for at-risk members and analyzing those data to fully understand a member’s clinical and nonclinical needs.
From there, healthcare providers can begin to develop a system that can leverage these types of data into their current healthcare delivery system and work toward clinical and social solutions that support holistic care.
-
Data Integration of Social Care into Healthcare Delivery
The third step to track the social determinants of health SDOH requires the data integration of SDOH and health equity. For this, the healthcare providers must focus on developing an infrastructure that integrates both clinical and social interventions. It’s not enough to only address clinical factors. For proper integration between SDOH and health equity, healthcare payers need to consider a broader approach. It must cover a myriad of social factors that influence their members’ well-being.
To address and solve this issue, every healthcare payer needs to evaluate the specific SDOH social determinants of the health needs of its members and accordingly work on the offerings of various health plans. To customize a good health plan, you can consider factors like where your members live, whether they have access to transportation, if they are experiencing food insecurity, etc.
Once those factors have been identified, SDOH and health equity can then work to identify and recruit the appropriate social service and community-based organizations in their members’ neighborhoods. These organizations will be the front-line supporters that will be able to help members address their nonclinical needs, such as bridging the gap in transportation issues or improving an issue of food insecurity. Once this network has been set up, health plans can oversee contracting, determine payment structures, and, finally, set up an infrastructure so that all components can work together seamlessly and holistically
-
Building an Accountable and Effective Network
Although few plans are currently addressing some of the major social determinants of health SDOH of its members, such as housing or transportation, some health plans still fail to cover the basic needs of its members.
Health plans that try to solve issues related to SDOH social determinants of health on their own often run into issues such as difficulty in prioritizing interventions or advocating for appropriate resources, inaccurate resource information, lack of accountability, fragmented coordination processes, and lack of transparency.
Conclusion
In essence, to properly implement SDOH and health equity, healthcare payers can ensure a thorough end-to-end infrastructure for their SDOH strategy—which includes relevant social service organizations. For instance, the patients must choose health plans from those organizations that have experience in gathering and analyzing data, recruiting social service organizations, managing the contracting process, implementing an infrastructure that supports seamless coordination, developing technology systems, and measuring the impact of social interventions.
When health plans form beneficial relationships with trusted SDOH health partners, they can more fully address the social needs of all members and promote more well-rounded health for all. Looking for a reliable platform that can provide medical updates in the healthcare industry?
Discover the latest payers’ news updates with a single click. Follow DistilINFO HealthPlan and stay ahead with the timely payer’s news updates. Join our community today!
FAQs
- What are Social Determinants of Health SDOH and why learning about them is important?
Ans: SDOH health conditions in which people are born, grow, work, live, and age, impacting their overall well-being. Knowing SDOH health is crucial because these social determinants continue to influence access to resources and opportunities in which they are brought up.
- How do Social Determinants of Health SDOH impact children and teenagers?
Ans: SDOH can lead to negative outcomes in mental health care among children and teenagers, such as failure in school, family conflict, violence, substance abuse, and even suicide.
- What strategies can healthcare payers implement to integrate SDOH and health equity for improved mental health outcomes?
Ans: Healthcare payers can integrate SDOH and health equity by understanding SDOH factors affecting their members, analyzing SDOH data, integrating social care into healthcare delivery, and building an effective network with social service organizations.