What Is an AI-First Healthcare System?
Artificial intelligence is no longer a futuristic concept in medicine. Today, AI tools actively support clinical documentation, image interpretation, risk prediction, patient triage, and remote monitoring. However, a fragmented, tool-by-tool approach is giving way to something far more ambitious — the AI-first healthcare system.
An AI-first model treats AI as core infrastructure, not a supplementary feature. Consequently, care delivery becomes proactive, coordinated, and data-driven across every touchpoint. Instead of deploying isolated tools, health systems build AI into every workflow — from the moment a patient books an appointment to the moment they receive post-discharge follow-up.
Moreover, industry analysts at PwC project that AI-driven, digital-first models could capture $1 trillion in annual healthcare spending by 2035, shifting care away from fragmented, brick-and-mortar facilities toward personalized, virtual-first systems.
Key Applications Driving the Shift
Clinical Documentation and Administrative Relief
Documentation and administrative tasks currently consume nearly twice as much clinician time as direct patient care. AI is rapidly changing this. Ambient AI tools now listen to patient-physician conversations and generate accurate clinical notes in real time. As a result, physicians spend less time on electronic health records after hours and more time on patient care and complex decision-making.
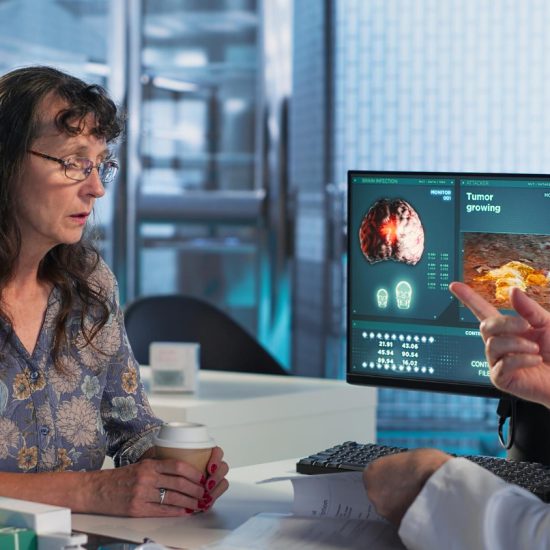
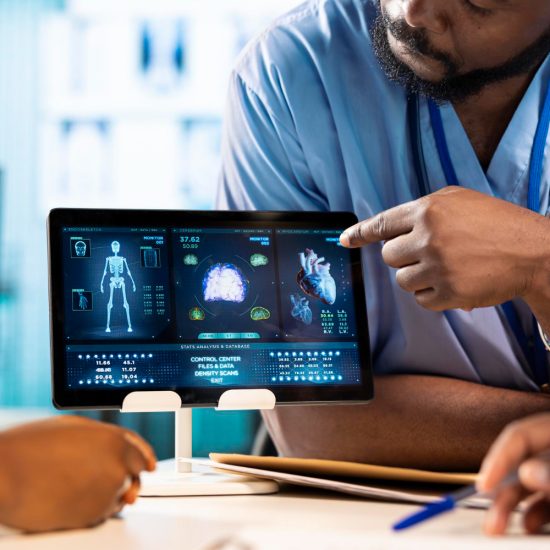
Diagnostic Imaging and Predictive Analytics
AI systems in radiology already match or exceed human performance on narrowly defined imaging tasks. Furthermore, these tools allow radiologists to handle higher clinical volumes and greater diagnostic complexity. Predictive analytics, meanwhile, help hospitals identify high-risk patients before conditions escalate — enabling earlier intervention at lower cost.
Patient-Facing AI and 24/7 Access
Patients increasingly turn to AI chatbots to research symptoms, review medications, and understand diagnoses. Therefore, patients now arrive at clinical appointments armed with AI-generated health information. Rather than viewing this trend as a threat, physicians should prepare for richer, more informed patient conversations. Additionally, AI-powered multilingual communication tools expand access for patients with limited English proficiency — making quality care available to underserved populations around the clock.
Barriers Standing in the Way
Despite clear momentum, several critical gaps slow down system-level AI integration.
Data Fragmentation and Interoperability
Health data sits in silos across hospitals, clinics, labs, and insurers. Without seamless interoperability, AI models lack the longitudinal, cross-setting data they need to deliver consistent value.
Algorithmic Bias and Equity Concerns
AI systems trained on historically unrepresentative datasets risk perpetuating health disparities. Therefore, equity-aware design must be a foundational requirement — not an afterthought — in any AI-first strategy.
Governance Gaps and Workforce Readiness
Many organizations treat AI governance as a compliance exercise rather than a strategic asset. Similarly, frontline healthcare workers often lack the training to use AI tools effectively. Consequently, early deployments fail to deliver promised returns on investment, eroding institutional confidence.
How Patients and Clinicians Must Adapt
The biggest shift is that AI will increasingly produce the first draft of clinical work — notes, summaries, and care orders — while clinicians focus on validation, interpretation, and decision-making. This is not a replacement of clinical judgment. Rather, it is an elevation of it.
For clinicians, the adaptation involves:
- Embracing ambient documentation to reduce EHR fatigue
- Engaging AI-informed patients as collaborative partners
- Using decision-support tools that extend beyond imaging into everyday care pathways
For patients, the shift means taking a more active role in their health. AI tools give patients greater access to information, but they also require greater health literacy. Therefore, patient education must evolve alongside AI adoption.
The Road Ahead for AI in Healthcare
Healthcare systems that move first will define the new standard of care. According to industry forecasts, 2026 marks a pivotal year — not just for AI pilots, but for scaled, integrated deployment. Systems that invested in AI governance, workflow integration, and staff training are already pulling ahead.
Furthermore, economic pressure is accelerating the timeline. Hundreds of hospitals face closure due to expiring ACA subsidies, Medicaid eligibility changes, and rising supply costs. This fiscal urgency pushes even the most cautious health systems to adopt AI faster — not as an innovation exercise, but as a survival strategy.
By 2035, physicians are expected to function as data orchestrators — using AI to triage risk, personalize care plans, and focus clinical energy on judgment and empathy. Hospitals, in turn, will shrink to high-acuity care nodes, while most routine care shifts into homes enabled by wearables, virtual command centers, and remote monitoring platforms.
The AI-first healthcare system is not a distant vision. It is, in fact, already taking shape. The question is no longer whether this shift will happen — it is whether health systems, clinicians, and policymakers are ready to lead it.