
Introduction: A Doctor’s Honest Reflection
Artificial intelligence is no longer a distant concept in medicine. Today, it sits at the center of how doctors diagnose, treat, and communicate with patients. Dr. Ashish K. Jha, former dean of Brown University School of Public Health and White House COVID-19 response coordinator, has watched AI tools like ChatGPT reshape his own clinical thinking. His conclusion? AI did not replace him. Instead, it made him a better doctor.
That shift in perspective is significant. Many physicians approach AI with skepticism. Yet, as real-world use grows, a new picture is emerging — one where AI and human expertise work together to improve patient outcomes.
From Skepticism to Openness
Dr. Jha describes entering the AI era with both cautious optimism and healthy skepticism. This balanced view reflects how most clinicians feel. On one hand, AI tools promise faster synthesis of medical data. On the other hand, errors in AI-generated advice carry serious consequences.
However, direct experience changed his thinking. When he began using AI to review complex patient histories, he noticed it catching details that time pressure often forced him to overlook. Furthermore, AI helped him translate dense clinical information into plain language — something patients deeply value. As a result, his consultations became clearer and more thorough.
How AI Is Changing Medical Practice
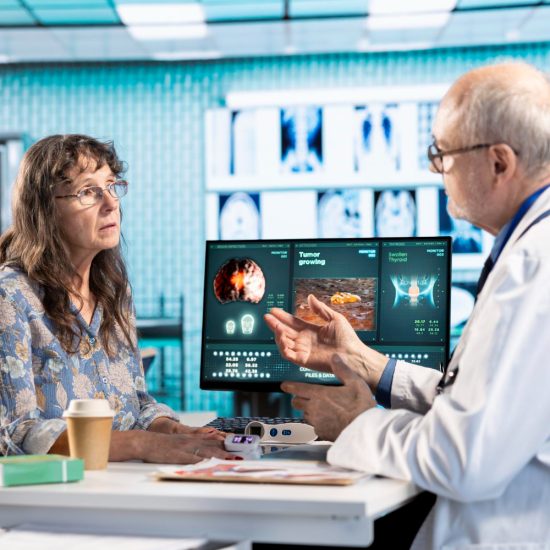
Smarter Diagnoses, Faster Decisions
AI systems excel at processing large volumes of information quickly. They consider full medical histories, overlapping conditions, multiple medications, and risk factors all at once. Doctors, by contrast, operate under tight time constraints. Consequently, AI fills critical gaps in clinical decision-making.
Stanford University now mandates AI training for all medical students. This move signals that AI literacy is becoming as essential as anatomy. Medical students today practice with AI-simulated patients, receiving real-time feedback on their questioning techniques and diagnostic reasoning. This kind of training was simply not possible before.
Additionally, AI reduces medication errors. Earlier generations of doctors had to memorize precise drug dosages by heart. Today, AI-assisted tools flag dangerous dosing errors before they reach patients — saving lives through automation.
Patients Are Already Using AI
Patients are not waiting for hospital approval. More than 230 million people worldwide ask health questions through ChatGPT every week. Roughly 40 million users turn to it daily for medical queries. Moreover, over one in three Americans have already used AI chatbots to research their health concerns.
This trend means patients arrive at consultations better informed. They bring AI-generated explanations of test results, coverage appeal letters, and targeted follow-up questions. Therefore, doctors must be prepared to engage with — and, at times, correct — AI-sourced information.
The Risks Doctors Must Acknowledge
AI carries real risks in healthcare. Some chatbots have been found to perpetuate outdated and racially biased medical assumptions. These errors can worsen health disparities, particularly for Black patients. Moreover, AI tools used in consumer settings often operate outside HIPAA regulations, raising important data privacy concerns.
Trust, therefore, is the central challenge. As one healthcare leader noted, the measure of AI’s success in 2026 is not simply whether it works — it is whether it can be governed, audited, and trusted. Doctors must remain the final safeguard in any AI-assisted clinical process.
What the Future of Healthcare Looks Like
The integration of AI into healthcare is accelerating at twice the rate of the broader economy. Yet only about 20% of healthcare organizations currently use it in meaningful ways. The pilot era is ending. What follows demands scalable, transparent, and human-centered AI deployment.
Looking ahead, AI will support earlier diagnoses, predict disease progression, and personalize treatment plans using real-time data. Tools like ChatGPT Health now allow patients to link their own medical records, lab results, and insurance documents directly to AI systems. This shifts the doctor-patient dynamic in important ways.
Ultimately, the vision is a system where humans and technology work together — not in competition, but in coordination. AI handles data synthesis and routine tasks. Doctors provide empathy, ethical judgment, and clinical accountability.
Conclusion: A Partnership, Not a Replacement
Dr. Jha’s experience offers a useful model for how physicians everywhere can approach AI. Resistance to change is understandable. Still, the evidence is mounting that thoughtful AI integration improves patient care. AI does not diminish the role of the doctor. Rather, it sharpens it.
The future of medicine belongs to those who learn to use these tools wisely — not those who fear them most.









Pingback: Focused Ultrasound Advances Brain Tumor Treatment / March 6, 2026
/
Pingback: New Nicotine Inhaler Trial Targets Smoking Cessation / March 6, 2026
/
Pingback: Innovaccer Highlights Healthcare AI Strategy at HIMSS / March 6, 2026
/